Diagnostic laparoscopy is a form of minimally invasive abdominal surgery that is performed to investigate potential sources of pelvic pain and infertility. During the procedure, the inside of the pelvic and abdominal cavities are carefully inspected for any abnormalities, such as endometriosis and adhesions. Diagnostic laparoscopy is typically performed under general anesthesia [1] and is commonly combined with therapeutic laparoscopy to treat any disease that is found.
What happens during the procedure?
First of all, the patient is put to sleep, her airways are intubated, her vital signs monitored and her bladder emptied with a catheter. The surgeon then performs a pelvic exam to check for any abnormalities. If a bladder condition is suspected (such as interstitial cystitis) a cystoscopy may be performed (the bladder is slowly filled with saline solution and a small camera is inserted to inspect the inside of the bladder for abnormalities). If abnormalities are suspected involving the inside of the uterus a hysteroscopy may be performed (a small camera is introduced through the cervix into the uterus to inspect the uterine cavity and obtain biopsies). An instrument called a uterine manipulator is then inserted through the cervix and into the uterine cavity. The uterine manipulator enables the surgeon to adjust the positioning of the uterus within the pelvis enabling complete visualization of the pelvic structures. Endometriosis often involves the tissue between the uterus and the large bowel (referred to as the Pouch of Douglas or the posterior cul-de-sac). In order to inspect this area during surgery, the uterus needs to be elevated forward.
After the placement of the uterine manipulator, a hollow needle is introduced to the pelvis through a tiny incision and the pelvic cavity is slowly insufflated (inflated) with CO2 gas. Normally the pelvic structures all rest together. The use of gas provides more space within the pelvis, separating the various structures and enabling visualization by the surgeon. Three small incisions are then made in the patient’s lower abdomen (these incisions are sufficient for both the diagnosis and treatment of endometriosis). One incision is made in the umbilicus (the belly button) and two are made beneath the bikini line, one on the right and one on the left. [2] After surgery the scars where these incisions were made will fade in time until they are barely noticeable and will be fully concealed by a bikini. A trocar (a cylindrical sheath through which the instruments are placed) is inserted through each incision. The laparoscope is introduced through the umbilical trocar (the trocar that is inserted through the patient’s belly button). A laparoscope is a thin fiber-optic tube with a camera integrated at the tip, which is connected to large video monitors so that the surgeon can inspect the inside of the pelvis. Surgical instruments are introduced through the other two trocars. These instruments may be used to grasp and move the pelvic structures, to irrigate (clean) surfaces, to suction (remove) free fluid from the bottom of the pelvis, and to dissect (separate) organs and structures that are fused together by adhesions (scar tissue) to allow the surgeon to inspect all surfaces.
The entire pelvic cavity is carefully examined with the tip of the laparoscope held close to the surface of the peritoneum (a thin layer of tissue that cloaks the pelvic structures). This enables the surgeon to detect any abnormalities, no matter how subtle. The pelvic structures, including the appendix, intestines, and diaphragm, are carefully examined for possible disease and adhesions. Any abnormalities in the appearances and consistency of the uterus are noted.
What are the challenges in identifying all areas of endometriosis?
The inside of the body is not like an empty room (where it’s easy to see if there is anything on the floor or walls). Instead, there are a lot of folds and nooks and crannies, and the search for endometriosis is more like trying to find a penny amongst a bunch of wadded up, unfolded cloths. With endometriosis, very small, difficult-to-see lesions can cause excruciating pain. When the end of the laparoscope is very close to the tissue, the laparoscope magnifies it. But this also decreases the area that is seen, similar to the effect of looking through a telescope or a set of binoculars.
A surgeon must be very thorough and meticulous, and use a systematic approach in looking for endometriosis. He or she also needs to understand the many different appearances of endometriosis, and work with an excellent pathologist who does not overlook mild endometriosis. The visual appearance of endometriosis is highly varied: The lesions can be dark, pigmented lesions, similar to a blood blister, or clear, vesicular lesions, appearing like miniature water balloons. It can also look like specks of salt or even leathery scar tissue. Some endometriosis is hard to see, but if the proper time and magnification are used, it can be found. In addition, scar tissue in an endometriosis patient should be considered and treated as endometriosis until proven otherwise.
The pathologist is an unseen and largely unappreciated member of the endometriosis team. If the pathologist is not meticulous in his or her examination of the tissue, then endometriosis will be missed, and the feedback to the surgeon will be false. Worst of all for the patient, the surgeon will leave endometrial lesions behind because the pathologist has incorrectly told the surgeon that this appearance is not endometriosis, when in fact it is. I work with a physician whom I believe to be one of the best endometriosis pathologists in the country. He has a lot of respect for endometriosis, and is very meticulous in looking for the disease. He takes extra steps in preparing the tissue, which helps to maximize the chance of finding all the endometriosis that is present.
Will diagnostic laparoscopy be proceeded by therapeutic laparoscopy?
After the pelvis has been carefully examined, the surgeon then proceeds to surgically treat any areas of suspected disease. The process of treating any abnormal findings is referred to as a therapeutic laparoscopy. Diagnostic and therapeutic laparoscopy are typically combined, although some surgeons first perform a diagnostic laparoscopy to assess the severity of the disease and then either plan in a further surgery to treat the disease or else refer the patient to a specialist. Dr. Cook always diagnoses and meticulously treats all areas of abnormal tissue during the same one procedure.
What happens once the surgery is complete?
Once the surgery is complete, the instruments and trocars are removed, the abdomen is carefully deflated and the incisions are glued or sutured closed and small dressings are applied. The patient is then taken to recovery and closely monitored. Anti-nausea and pain meds are provided via IV to keep the patient comfortable. Following surgery Dr. Cook admits his patients overnight so that they receive optimal management of their post-operative pain. During the first hours following surgery you may feel groggy and tired and your throat may feel sore from the intubation tube. The fatigue may last for some days to several weeks, depending on the length of surgery and your physical condition prior to surgery. In most cases any post-operative pain is well managed by the IV, PCA pump and orally administered pain medications while in hospital and the pain medications prescribed following discharge. Residual gas from the surgery may take some time to dissipate, causing temporary shoulder tip pain but usually resolves within a few days. Likewise, the incision sites may be tender and bruised for the first week or two after surgery but will recover in time. Slowly you will find yourself returning to your normal activities. The length of recovery will depend on the patient’s general health as well as on the extent of surgery that has been required.
Dr. Cook and his team carefully follow up all surgery patients to make sure they are comfortable and recovering well. If any concerns arise, the Vital Health team is on hand to help you.
How effective is a diagnostic laparoscopy at identifying endometriosis?
In the capable hands of an endometriosis specialist diagnostic laparoscopy is a highly accurate method of identifying any abnormal tissue and confirming the presence or absence endometriosis. Surgeons who are less familiar with endometriosis, however, may fail to recognize subtle areas of disease and may misinterpret the clinical significance of dense adhesions (which to a specialist is often a sign of significant underlying invasive disease). An unfortunate outcome is where a patient with endometriosis is incorrectly told by her surgeon that she does not have the disease, further delaying correct diagnosis and treatment. It takes a trained eye to recognize endometriosis in all its forms and make an accurate diagnosis. It is therefore important to request that your surgeon documents the surgery by taking photos and/or providing you with a complete digital copy of your procedure on DVD. This way, you can seek a second opinion if you suspect disease has been missed. Ideally, it is best to find an endometriosis surgical specialist to conduct your surgery. Dr. Cook records all of his surgeries and provides his patients with comprehensive surgical photos and a complete copy of the procedure on DVD on request.
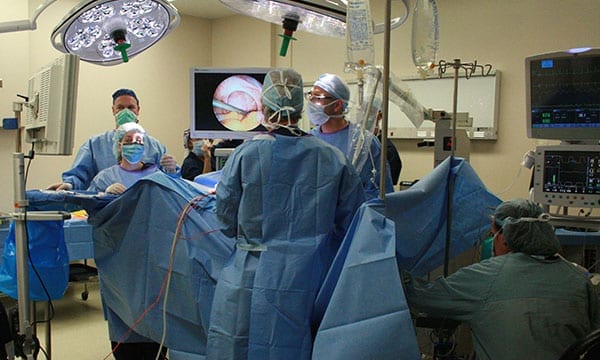
Dr. Cook and his team performing a diagnostic laparoscopy.
Notes
- Occasionally patient-assisted laparoscopy (PAL) will be performed, in which the patient is awake during the procedure and can guide the surgeon to the source of her pain. PAL may be indicated if previous laparoscopic surgery has failed to identify and resolve the patient’s pain.
- In patients with symptoms suggestive of diaphragmatic endometriosis an extra incision may be required in the upper right quadrant of the abdomen (just under the right rib margin) in order to fully visualize the right side of the diaphragm behind the liver.