Interstitial cystitis (IC) is a chronic bladder condition that often mimics a bladder infection. While the cause is generally unknown, several precipitating events have been identified as potentially triggering the condition, including trauma to the bladder, bladder over-distention, pelvic floor dysfunction, and hypersensitivity or inflammation of the pelvic nerves.
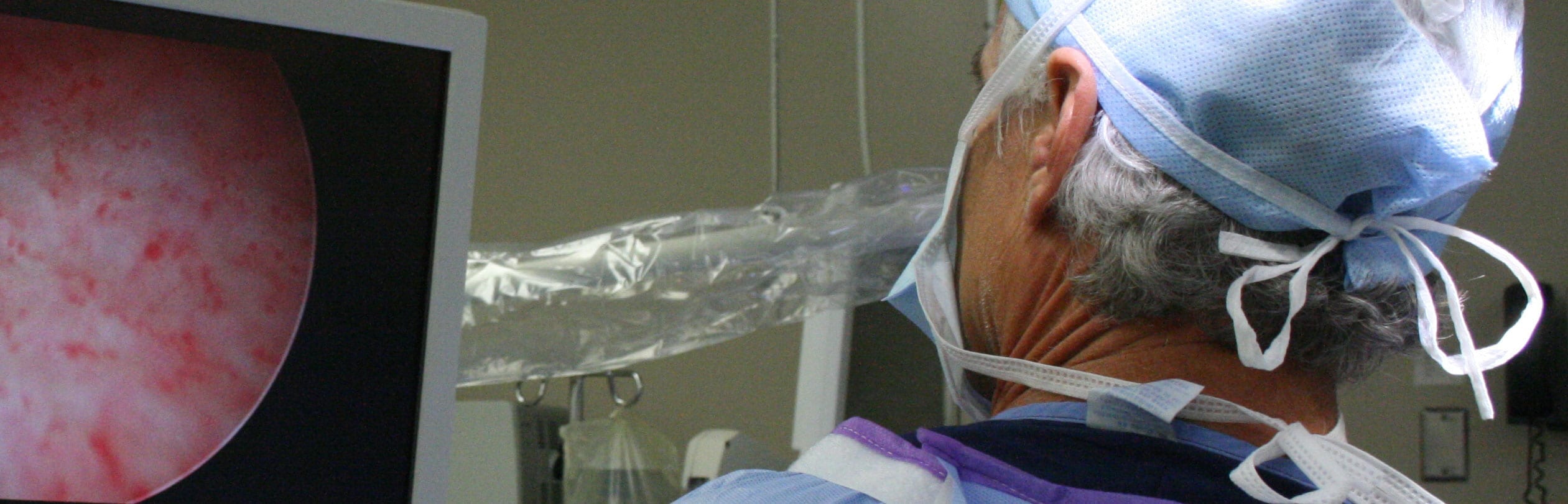
Patients with IC typically have a smaller bladder capacity and when the inside of the bladder is inspected via cystoscopy (a special tiny camera introduced into the bladder), glomerulations (small capillary bleeding from the bladder wall) and Hunner’s ulcers (lesions or sores on the lining of the bladder) may be observed (Hunner’s ulcers affect approximately 5-10% of patients who have IC).
- Urinary frequency – a need to urinate many times during the day and/or night
- Urinary urgency – a sensation of having to urinate urgently. Urinary urgency may be accompanied by a feeling of pressure or pain in the area of the bladder
- Pelvic pain, pressure and discomfort in the bladder, urethral and vaginal region
- Pain during sexual intercourse
A diagnosis of IC may initially be suspected based on your symptom history and on a questionnaire assessing bladder pain, and urinary frequency and urgency. The next step toward diagnosis is to rule out any other possible diagnoses that could explain these symptoms.
Commonly used tests:
- Pelvic exam (to assess for the location of any tenderness)
- Lab testing (to rule out chronic urinary tract infection)
- Urodynamics (to assess bladder, urethra and sphincter muscle function)
- Potassium sensitivity test (an infusion of potassium chloride is introduced into the bladder while the patient is conscious. If the patient experiences pain, this can be indicative of IC although the test has been criticized for its poor level of test reliability)
- Cystoscopy and hydrodistention (with the patient under general anesthesia, a catheter is placed in the bladder and the bladder is slowly filled with saline solution to measure bladder capacity, and a cystoscope is used to inspect the inside of the bladder for any abnormalities)
While there is no curative treatment for IC, there are treatments available to help manage symptoms and improve quality of life. The treatments indicated will depend in part on the suspected cause of your bladder pain.
Treatments include:
- Dietary changes
- Self-management (bladder retraining and relaxation techniques/stress management)
- Medical therapies to reduce pain, tissue reactions and inflammation and bladder spasm
- Physical therapy if pelvic floor dysfunction is a contributing factor
- Neuromodulation – use of nerve stimulators to help manage urinary function
- Bladder instillations (medications introduced into the bladder via catheter)
- Removal or destruction of Hunner’s ulcers during cystoscopy
IC has been found to be common in patients with endometriosis and other pelvic pain disorders, and for this reason, is often referred to as the “evil twin” of endometriosis. At Vital Health Endometriosis Center, our IC patients benefit from the full range of western and integrative treatment modalities, from the specialized management of medical therapies and minimally invasive therapeutic interventions to customized nutritional counseling to reduce pain flares and daily symptoms. While there is no definitive cure for IC, with the right combination of treatments our IC patients can expect significant relief from this debilitating condition.
