At the Vital Health we have successfully treated hundreds of patients with severe adhesions, and for some their surgery was not only life changing but life saving. Our adhesion patients are offered the same ongoing follow-up care as our endometriosis patients.
What are adhesions?
Adhesions are bands of scar tissue that form between adjoining organs and structures, causing them to fuse together. Adhesions can be thin like cobwebs or thick and dense like hardened glue. Adhesions can result from disease (such as endometriosis), infection (such as pelvic inflammatory disease), injury (such as following abdominal surgery) or may have no known cause (idiopathic adhesions).

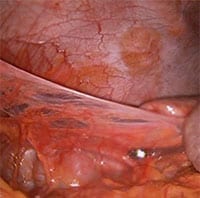 When pelvic adhesions occur they can cause a range of symptoms depending on the organs and tissues that are involved. If the ovaries are involved by scarring or are adhered to the pelvic side walls, the presence of a cyst in the ovary can cause the adhesions to stretch, resulting in a painful, pulling sensation. If the intestines are involved by adhesions, this may result in severe cramping pains due to restricted motility of the gut, and if a section of bowel is constricted by an adhesion, partial or complete bowel obstruction can result, causing severe pain, nausea, and vomiting, constipation, and diarrhea. In severe cases of adhesions, the pelvis may become “frozen” by extensive dense adhesions, fusing the bladder to the uterus, the uterus to the large bowel, and the ovaries and tubes to the bowel, pelvic sidewalls, and uterus. In rare cases the entire abdominal cavity, containing the reproductive organs and intestines, will be obliterated by severe adhesions, distorting the pelvic anatomy and making it impossible for the surgeon to identify the pelvic organs without first conducting an extensive and painstaking dissection of the adhesions.
When pelvic adhesions occur they can cause a range of symptoms depending on the organs and tissues that are involved. If the ovaries are involved by scarring or are adhered to the pelvic side walls, the presence of a cyst in the ovary can cause the adhesions to stretch, resulting in a painful, pulling sensation. If the intestines are involved by adhesions, this may result in severe cramping pains due to restricted motility of the gut, and if a section of bowel is constricted by an adhesion, partial or complete bowel obstruction can result, causing severe pain, nausea, and vomiting, constipation, and diarrhea. In severe cases of adhesions, the pelvis may become “frozen” by extensive dense adhesions, fusing the bladder to the uterus, the uterus to the large bowel, and the ovaries and tubes to the bowel, pelvic sidewalls, and uterus. In rare cases the entire abdominal cavity, containing the reproductive organs and intestines, will be obliterated by severe adhesions, distorting the pelvic anatomy and making it impossible for the surgeon to identify the pelvic organs without first conducting an extensive and painstaking dissection of the adhesions.